The ‘Big Beautiful Bill’ Was a Big Beautiful Bust for Telehealth, and Now the Clock Is Ticking

While President Trump’s reconciliation package did reinstate first-dollar coverage for HDHP-HSAs, a collection of waivers aimed at boosting coverage for and use of telehealth didn’t make the cut.
Over 200 Organizations Call on DEA to Continue Remote Prescribing of Controlled Substances

The Alliance for Connected Care, the American Telemedicine Association and numerous other organizations sent a letter to the DEA urging action to safeguard remote prescribing of controlled substances.
Medicare telehealth use: High satisfaction, low future interest

A federal report details the latest telehealth use trends within the Medicare program, showing high satisfaction with the services, but lower interest in continued access to telehealth.
Abortions Accessed Through Telemedicine Are Growing Despite Legal Challenges

Three years after the Supreme Court overturned Roe v. Wade, abortions in the U.S. are on the rise due to provider shield laws
UAMS study says virtual care helps close postpartum gaps
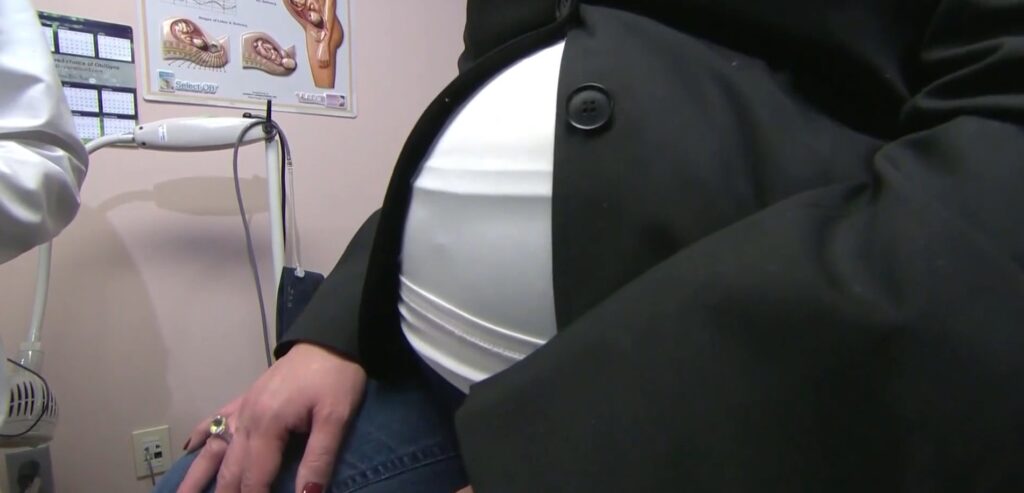
A new UAMS study finds that virtual postpartum care can increase critical health screenings for new mothers.
Military health system looks to AI, virtual care for battlefield readiness

The military health system is already deploying virtual healthcare capabilities that allow specialists to provide remote consultation to battlefield medics.
Virtual Health Coaches: The Future of Personalized Anti-Aging Programs

Virtual health coaches represent a paradigm shift in how we approach aging and wellness.
To improve virtual care use, why HR should turn to behavioral science

Health plan members can achieve better health and lower medical costs with primary care, but only if they have adequate access to primary care clinicians. The United States is in the midst of a severe primary care shortage. A recent survey found that primary care appointment wait time is 23.5 days, an increase of 14% over the past three years.
How telehealth is connecting the unhoused to care in SC

MUSC Health’s hybrid CARES program expands access to unhoused individuals, leveraging telehealth and street medicine to reduce barriers to care like transportation.
How AI is changing telemedicine in 2025
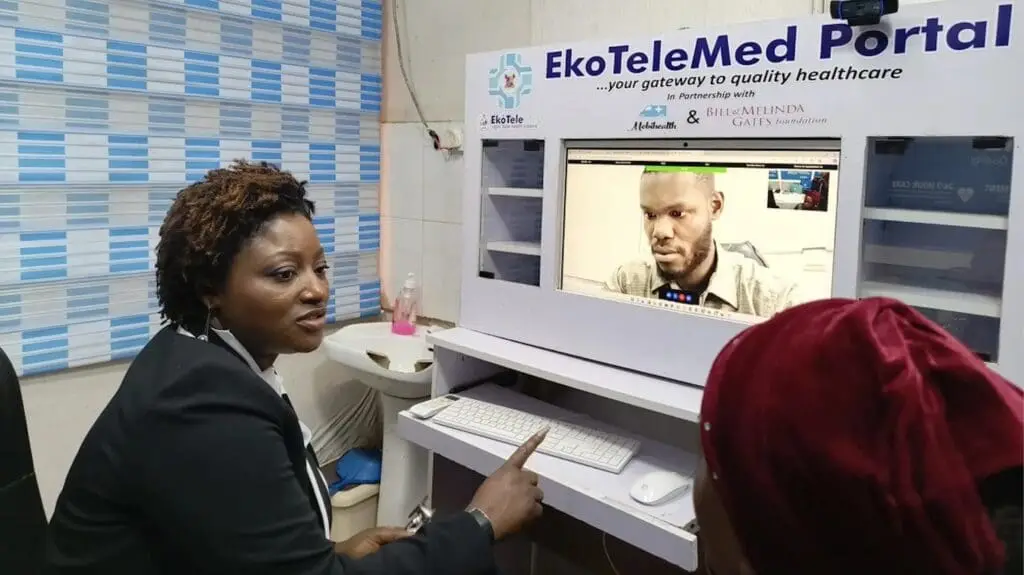
AI is virtually expanding, reshaping and personalizing telehealth practices in triaging, image analysis, patient diagnoses, treatment planning, monitoring and mental health.
